Can You Actually Reverse Your Biological Age with Diet? What a New 4-Week Study Found
The Short Version
- University of Sydney researchers found that four weeks of plant-based, lower-fat eating produced measurable improvements in epigenetic aging markers — biological age moved faster in response to diet than most research windows expect to capture.
- Biological age, measured through DNA methylation patterns, is a better predictor of disease risk than chronological age — and unlike your birthday, it can shift in either direction based on lifestyle.
- Women at 50 who followed four or five healthy lifestyle habits lived 34 disease-free years afterward, versus 24 for those who followed none — a 10-year difference in healthy life that Harvard's research attributes substantially to diet and movement.
- High adherence to the MIND diet was associated with a 53% reduced rate of Alzheimer's disease in a study of 923 older adults; even moderate adherence produced a 35% reduction.
- Loneliness is associated with a 57% increased early mortality risk — which means who you eat with may matter as much to your biological age as what ends up on the plate.
- Dietary patterns — Mediterranean, MIND, DASH — consistently outperform individual superfoods in longevity research because the body responds to the cumulative eating environment, not single ingredients.
Four weeks. That is what researchers at the University of Sydney gave older adult participants to answer a question a lot of people are quietly asking: can diet actually reverse biological age? In a study published in May 2026, participants who shifted toward plant-based, lower-fat eating appeared biologically younger on epigenetic aging measures by the end of the intervention. Not dramatically. But measurably — in a direction that matters.
What you put on your plate is doing something. That has always been true. What is new is that we can now watch it happen at the level of your DNA.
What Biological Age Actually Means (And Why It Is Different from Your Birthday)

What Biological Age Actually Means (And Why It Is Different from Your Birthday)
Your chronological age is the number of years since you were born. Your biological age is something different — an estimate of how old your cells and tissues actually function, as measured by markers that track physical wear and repair. Two people who are both 60 years old chronologically can have biological ages that differ by a decade or more, depending on genetics, lifestyle, and — increasingly, the research shows — what they eat.
The most reliable tools for measuring biological age are called epigenetic clocks — algorithms that read patterns in how DNA is chemically tagged, specifically through a process called DNA methylation. These chemical tags act like dimmer switches on genes, influencing which ones are active and which are silenced. Over time, methylation patterns drift in ways that correlate predictably with aging and disease risk. Scientists can now estimate biological age from a blood or saliva sample with remarkable accuracy — and the number they get often differs meaningfully from the one on someone's driver's license.
Why does this matter? Because biological age appears to be a better predictor of disease risk and mortality than calendar age. Two people who share the same birthdate can have meaningfully different risks of heart disease, cognitive decline, and cancer — and epigenetic measurements capture more of that variance than birth year alone. It is, in effect, a report card on how your body is aging.
The promising part is that epigenetic patterns are not fixed. They are influenced by what you eat, how you sleep, how much you move, and whether you are under chronic stress. They can shift — in both directions. The dietary patterns that support that shift are not exotic or expensive. Here is what the research shows those patterns actually look like:
What the New University of Sydney Study Actually Found

What the New University of Sydney Study Actually Found
The study design was practical, not extreme. Older adults participated in a four-week dietary intervention that shifted their eating toward more plant-based foods and reduced overall fat intake — a realistic change rather than a clinical elimination protocol. Before and after the intervention, researchers measured epigenetic aging markers, looking specifically at how participants' DNA methylation patterns had shifted.
The result: those who followed the dietary shift appeared biologically younger at the end of four weeks on those epigenetic measures, compared to their baseline at the start. What the study measured was not weight or cholesterol — the standard metrics most nutrition trials chase — but the biological age markers themselves. That makes the finding more direct than most food-and-health research.
The mechanism is not fully understood, but the pattern is consistent with what the anti-inflammatory diet literature has documented for years: eating more whole plants and less saturated fat creates conditions in which cellular repair outpaces cellular damage, at least in the short term. When that happens, the methylation patterns that epigenetic clocks read shift in a favorable direction.
What does it mean that a four-week change in what you eat leaves a measurable trace in your DNA?
Which Foods Have the Strongest Evidence for Slowing Biological Aging

Which Foods Have the Strongest Evidence for Slowing Biological Aging
The research does not point to a single superfood. It points to patterns — and within those patterns, certain food categories show up consistently enough across independent studies to be worth naming directly.
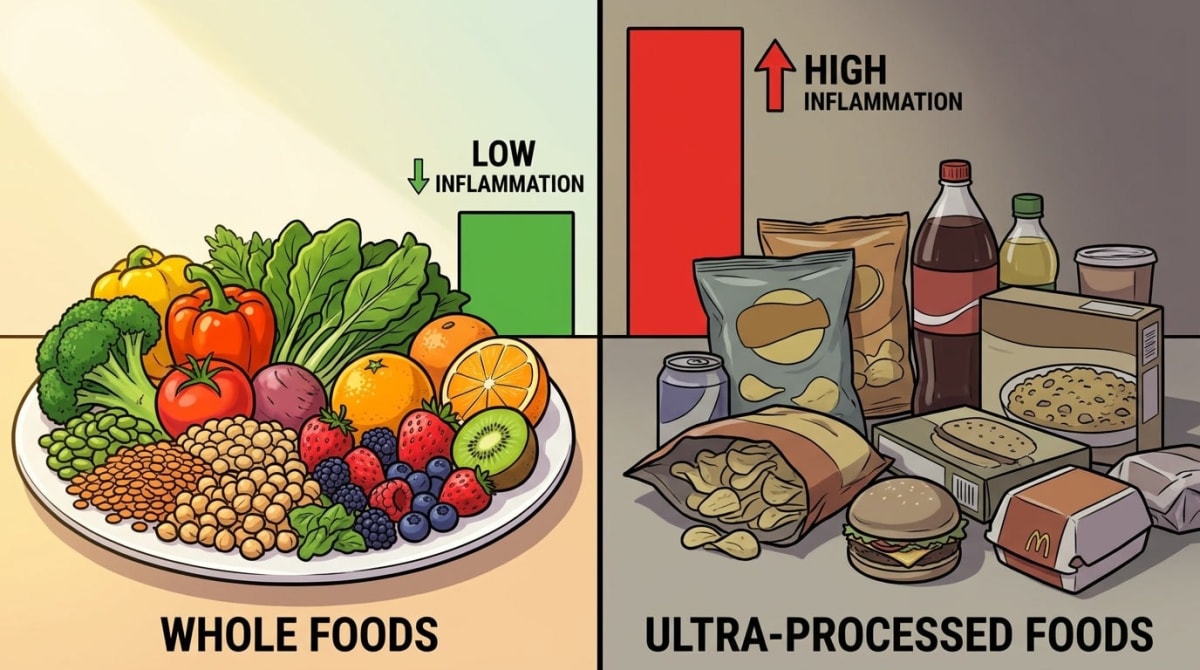
Whole plants — vegetables, legumes, fruits — are the most consistent finding across longevity research. They carry fiber, polyphenols, and antioxidants that reduce oxidative stress, one of the primary drivers of epigenetic aging. A meta-analysis of 17 studies found that vegetarians had consistently lower C-reactive protein levels than omnivores. C-reactive protein is a primary marker of systemic inflammation — and chronic low-grade inflammation is one of the most reliable predictors of accelerated biological aging.
Olive oil and omega-3 fats work through anti-inflammatory mechanisms. According to Harvard's Nutrition Source, a Mediterranean diet significantly decreased several inflammatory markers compared with a low-fat diet in randomized trial data. Omega-3s, found in fatty fish, walnuts, and flaxseed, appear to directly reduce inflammatory signaling at the cellular level — the same level where epigenetic aging markers respond.
ultra-processed foods are the flip side. Research published in journals including Cell Metabolism has documented their association with accelerated epigenetic aging, likely through inflammatory additives, refined carbohydrates, and the displacement of whole foods that would otherwise support cellular repair. The mechanism is the inverse of what plant-based data shows: ultra-processed eating creates conditions where cellular damage accumulates faster than it is repaired.
The Diet Patterns with the Best Longevity Track Records

The Diet Patterns with the Best Longevity Track Records
Individual foods tell part of the story. What the evidence actually shows working — at the level of health outcomes measured over years and decades — is dietary patterns, not single ingredients.
Three patterns appear consistently at the top of longevity research: the Mediterranean diet, the MIND diet, and the DASH diet. They share more than they differ. All three are built on whole vegetables, legumes, whole grains, fish, and olive oil. All three limit red meat and ultra-processed foods. All three have been tested in randomized controlled trials and large observational cohorts with consistent findings on inflammation, cognitive aging, and cardiovascular risk.
The MIND diet data for brain aging is particularly striking. According to Harvard's Nutrition Source, among 923 older adults studied over years, those who most closely followed the MIND diet showed a 53% reduced rate of Alzheimer's disease. Even moderate adherence showed a 35% reduction. Those are meaningful numbers for any dietary intervention.
Why do patterns outperform individual foods? Because the body responds to the cumulative environment across meals and days, not single ingredients. Olive oil and leafy greens eaten alongside processed meat and refined flour will not produce the same inflammatory profile as those same foods within a coherent Mediterranean pattern. The whole eating environment matters — what you surround your good choices with shapes what those choices actually do.
What Four Weeks of Eating Differently Can Actually Do

What Four Weeks of Eating Differently Can Actually Do
Four weeks is a short window. Finding meaningful epigenetic change in that window is significant — but it is worth being precise about what changes fast and what changes slowly.
Inflammation markers respond quickly. C-reactive protein, interleukin-6, and other inflammatory markers can shift measurably within two to four weeks of meaningful dietary change. This is the mechanism most likely driving the epigenetic age improvement the Sydney researchers found: when inflammation drops, cellular conditions for repair improve, and the methylation patterns that epigenetic clocks read shift in a favorable direction.
Structural aging changes more slowly. Telomere length, organ-level cellular composition, and other deeper markers of biological age respond over months and years, not weeks. Four weeks of plant-heavy eating is not a permanent reset. It is a demonstration that the markers are movable — and a beginning.
Consistency past four weeks is what matters. The Harvard healthy longevity research quantifies this directly. According to Harvard T.H. Chan School of Public Health, women at age 50 who practiced four or five healthy lifestyle habits — including a diet aligned with Mediterranean or DASH patterns — lived approximately 34 additional years free of diabetes, cardiovascular disease, and cancer. Those who practiced none lived approximately 24 disease-free years. The difference is a decade of healthy life.
The starting point that works is not perfection. It is one or two meals a week shifted toward more plants, better fats, and less processed starch. Most people who successfully change their eating over time don't change everything at once — they change something consistent and let that become normal.
What to Put on Your Plate This Week

What to Put on Your Plate This Week
The research is clear enough to translate. Here is what it points to, without the optimization spiral:
Legumes at least three times a week. Lentils, chickpeas, black beans — any form. They appear in every longevity diet pattern, consistently, across populations. They carry fiber, polyphenols, and protein in combination. A salad with chickpeas instead of croutons, a lentil soup that lasts three meals — either one is a meaningful shift that requires no special equipment or planning.
Olive oil as your primary cooking fat. Not as a supplement — as the thing you reach for when you cook. The Mediterranean trial data showing decreased inflammatory markers compared to low-fat diets is about olive oil as a dietary constant, not an occasional addition.
More fish, less processed meat. The MIND and Mediterranean patterns include fatty fish — salmon, sardines, mackerel — for their omega-3 content. Processed meat is consistently associated with accelerated aging outcomes in the literature. Reducing it is one of the highest-leverage changes the research points to.
More vegetables at every meal, without turning it into a project. The research doesn't care whether they're raw or roasted, exotic or common. It cares about volume and consistency. A meal that is half vegetables — in a soup, roasted alongside a protein, in a grain bowl — moves the pattern in the right direction.
Less ultra-processed food as a default, not a rule. The goal is not to never eat a chip. It is to make whole food the background of your eating rather than the exception.
And here is what the Harvard five-factor data makes explicit, because it is easy to miss: loneliness is associated with a 57% increased risk of early mortality. That puts the dinner table in a different frame entirely. The meal is not just fuel. Who you are eating with — whether there is any care in the preparation, whether there is conversation — may be doing as much as any single dietary choice.
This research is not an invitation to anxiety about every food choice. It is confirmation that what most people who eat well already know intuitively is right: real food, eaten consistently, prepared with some care, shared where possible, does something. It turns out that something is now measurable. It shows up in DNA methylation patterns after four weeks. It shows up in disease-free years after fifty.
What would it look like to add one more real meal to your week?


